Exercise and Chronic Pain

Chronic pain is perhaps the most pervasive medical issue in the United States. The longterm impacts of chronic pain often cause individuals to reduce or eliminate physical activity. Chronic pain is generally defined as any pain that lasts longer than expected healing time, but typically the label “chronic” is applied when pain continues longer than three to six months (Treede et al., 2015). It is estimated that 20% of adults in the U.S. experience chronic pain, with an additional 8% of adults experiencing frequent, and at times debilitating, chronic pain (Geneen et al., 2017). In fact, chronic pain is the most common reason adults seek medical treatment in the United States (Geneen et al., 2017).
Chronic pain can impact physical, mental, and emotional well-being, which can limit daily activity and quality of life. This impact on wellbeing ranges in severity from moderate to severe (Dueñas et al., 2016; Geneen et al., 2017). The purpose of this fact sheet is to address the common barriers to being physically active with chronic pain and provide suggestions for safe ways to be physically active even when chronic pain is present.
How Does Chronic Pain Impact Activity?

One way of measuring pain is interference with normal daily activity. Chronic pain conditions can seriously affect daily activities and quality of life (Amtmann et al., 2010; Dueñas et al., 2016). Some of the ways pain has been shown to limit activity (Björnsdóttir, et al, 2013; Henschke, et al., 2021) include the inability to:
- Carry groceries.
- Climb stairs.
- Stand up straight.
- Maintain energy by the end of the day.
- Continue activities or continue without rest breaks.
- Uphold schedules, missing school or work.
- Sustain sociability, withdrawing from activities.
One study in the U.K. found that approximately 70% of all neck pain moderately to severely limited the amount and types of daily activity (Thomas et al., 2004). Worse yet, mental health generally declines as the pain intensifies (Gilmour, 2015).
In the past, pain assessments focused solely on pain intensity and location. Doctors now recognize that fully understanding pain’s impact means researchers must measure the emotional and behavioral impacts and how pain interferes with physical functioning (Breivik et al., 2008).
How Do the Body and Mind Respond to Pain?
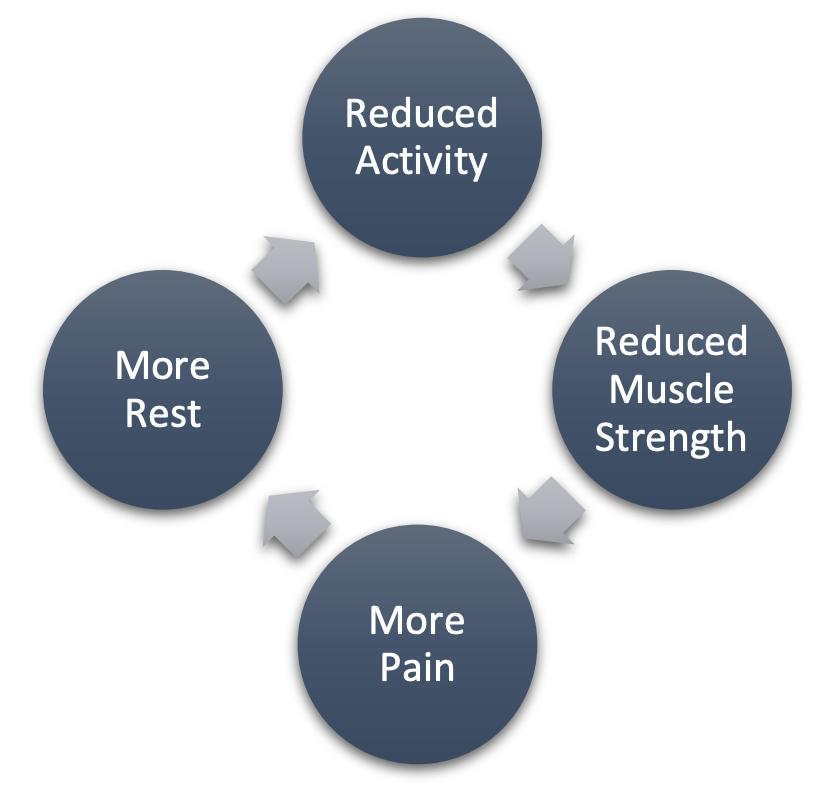
When an individual suffers from chronic pain, the natural response is doing anything to reduce it. For many, that instinct is to rest and relax. This response can initiate a vicious cycle of self-limiting activity, shown in Figure 1 (Grady & Gough, 2014).
Too much rest can be detrimental and result in atrophy (or wasting) of the muscles, leading to further health problems, including poor posture, less joint stability, and other structural problems (Loos et al., n.d.). The reasons we may limit physical activity are easy to understand using the “fear-avoidance” model of pain. We avoid activity because we fear injury or pain from movement. When we stop, rest, or avoid movement, we feel less afraid, and that sense of relief reinforces the decision to stop the activity. This cycle eventually increases the level of disability and distress (Mackichan et al., 2013).
Activity restriction can become so limiting that chronic pain sufferers feel their independence is threatened because of their pain (Mackichan et al., 2013). While these reactions are understandable, all of the evidence points toward the benefits of physical activity in managing pain.
How Does Activity Benefit Chronic Pain Sufferers?

Studies show many general health benefits of physical activity, including boosts to brain health, weight management, reduced disease burden, and stronger bones and muscles (Center for Disease Control and Prevention [CDC], n.d.). The CDC even notes that maintaining a physically active lifestyle reduces the risk of developing chronic diseases such as heart disease, diabetes, hypertension, some forms of cancer, and other obesity-related illnesses.
Physical activity can lower the risk for developing chronic pain and assist in managing existing chronic pain (Law et al., 2017). Individuals suffering from chronic pain can enjoy a number of benefits of physical activity and exercise. Physical activity reduces chronic pain by building muscle strength and flexibility, reducing fatigue, reducing pain sensitivity, and reducing inflammation. Research suggests that exercise may even be effective in reducing pain for difficult-to-treat conditions like fibromyalgia and neck/shoulder pain (Belavy et al., 2021). Physical activity also provides the following additional benefits.
Builds muscle strength. Physical activity can help prevent muscular atrophy, which decreases pain by strengthening the muscles and improving flexibility (Law et al., 2017).
Reduces fatigue. Physical activity has been shown to reduce fatigue, a common symptom in many chronic pain conditions (Rall et al., 2011).
Improves sleep. A meta-analysis of highquality research indicated significant improvements in sleep quality (Ambrose & Golightly, 2015).
Reduces pain sensitivity. Some research has found that exercise may be effective for reducing pain sensitivity compared to nonexercise training treatments (Belavy et al., 2021). Exercise can change how the brain responds to pain by normalizing the pain signal process and promoting the release of analgesics, such as natural pain relievers and serotonin, that turn off pain signals (Law et al., 2017).
Reduces inflammation. Muscles can release chemicals that prevent pain signals from going to your brain, and the immune system increases anti-inflammatory cytokines that promote tissue healing (University of Iowa, 2018).
Reduces depression and anxiety and improves mood. With 80–90% of chronic pain sufferers experiencing mood disruption due to their pain, the benefits of physical activity are worth considering (Ambrose & Golightly, 2015).
The CDC produced a chart summarizing the multiple health benefits of physical activity: https://www.cdc.gov/physicalactivity/basics/adu lts/pdfs/Health_Benefits_PA_Adults_Jan2021_ H.pdf.
Is Physical Activity Right for Me?
Recent research recommends that because physical movement is so important in improving chronic pain, doctors should prescribe it to patients, similar to how they prescribe medications (Sanchis-Gomar et al., 2021). Both aerobic and strengthening exercises can help reduce or manage pain. The important thing is to keep moving. When determining the best exercise for you, choose exercise that you enjoy. This will help you continue to be active.
Doctors have not come to a consensus on how much exercise to recommend based on different chronic pain conditions. The general recommendation is that movement, no matter how minimal, is desirable. Added to this are four precautions that can make exercise safe for almost any condition: (1) Modify to reduce risk of falls; (2) Ensure proper posture; (3) Use a range of motion that doesn’t increase pain; and (4) Use a “start low, go slow” approach (Ambrose & Golightly, 2015).

A healthcare professional can review your current health status, activity level, and prior health-related events using the Physical Activity Readiness Questionnaire (PAR-Q) (Harvard Medical School, 2012). This tool can help assess your readiness to engage in physical activity (Warburton et al., 2011; Bredin et al., 2013). Find the updated 2017 version at https://store.csep.ca/pages/getactivequestionn aire (Canadian Society for Exercise Physiology, 2021).
Despite the many benefits of physical activity, it can still feel overwhelming to contemplate increasing physical activity when suffering from chronic pain. It is important to note that being physically active does not have to involve a gym membership, formal exercise classes, or vigorous-intensity activities. Engaging in any activities that result in moving more and sitting less will lead to the desired health benefits and possibly help manage or reduce your chronic pain (U.S. Department of Health and Human Services, 2018). Figure 2 displays activities that might work well for individuals with chronic pain.
Figure 2. Activities for Individuals With Chronic Pain
Endurance
- Walks in your community.
- Low-impact activities like swimming or bike riding.
- Tasks around the house like sweeping, vacuuming, and dusting.
Strength Building
- Lifting items found around the house.
- Seated strength training exercises.
- Exercise bands.
Flexibility/Stiffness
- Stretching activities.
- Tai chi.
- Yoga.

While being physically active can lead to overall health benefits and management of chronic pain, pacing is important to avoid overdoing it (Grady & Gough, 2014). The vicious cycle of overdoing begins as a person begins to recover, feels better, then pushes too hard, resulting in more pain and eventual collapse and a longer recovery. As you contemplate whether to increase your activity, the National Institutes on Aging (n.d.) offers these suggestions to avoid pushing your body too hard:
- When being physically active, do not ignore worsening pain. Ignoring pain can exacerbate pain conditions and possibly lead to inflammation.
- Avoid pushing your body too hard on days where your chronic pain is less intense. Even though you may be feeling better, it is still important to not overdo it.
- If pain, swelling, or inflammation is present in a specific joint or body area, focus on a different area.
- If pain increases or something does not feel right in your body, seek advice and support from your medical team.
How Do I Get Started?
If you haven’t been active before, or are becoming active again after a long break, consider these tips as you make a plan:
- Access an expert. Consult with a physician or medical professional about starting or re-engaging in activity.
- Personalize guidelines. Don’t let the guidelines get you down. Although the general physical activity recommendation for adults is 30 minutes per day, five days per week (totaling 150 minutes), studies show that breaking up exercise sessions into 10-minute chunks has similar health benefits (Harvard Medical School, 2018). Research shows that moderate activity just two to three times a week reduces pain and depression (Ambrose & Golightly, 2015).
- Include routine activities, chores, and hobbies. Physical activity includes any activity that increases movement and decreases sedentary time. Practical suggestions adapted from the CDC (2021) and others for incorporating daily physical activity follow.
- Dedicate time to make activity part of the day, and consider it an appointment, just like a doctor’s appointment.
- Consider activities, locations, and times that are enjoyable and motivating.
- Engage your family and friends to act as motivators for one another.
- Start slowly and work up to more challenging activities. Rushing into an activity can lead to soreness, fatigue, injury, and loss of motivation to continue.
- Break up bouts of sitting by standing and doing activities, such as marching during TV commercials, walking around the office, and walking up and down stairs (Harvard Health Publishing, 2014).
- Interrupt sitting with activities to improve glucose levels, insulin response (Dunstan et al., 2012), resting blood pressure (Larsen et al., 2014), fatigue, and musculoskeletal discomfort (Thorp et al., 2014).
- Consider costs. Examine any potential costs of starting a physical activity program and choose options within your budget.
- Modify classes to meet needs. Ask to join exercise classes during the warm-up or cool-down periods only if whole sessions are too strenuous.
- Use alternate resources. Find physical activity routines on the internet, TV, and other online resources.
- Use promotions. Use trial periods and local programs to increase options. Consider the following examples.
- Take advantage of free trial periods and multiple facilities, noting equipment quality, safety, trained staff, hours, busy times, etc. (American College of Sports Medicine [ACSM], 2019).
- Watch out for fees and promotional periods that may be incorporated into membership plans and negotiate for better terms (ACSM, 2019; American Council on Exercise [ACE], 2009a).
- Utilize free sessions with a personal trainer offered with gym or facility memberships and ask additional questions to learn about the equipment and the trainer to determine whether the relationship is a good fit (ACE, 2009b).
How Do I Overcome Barriers?

Barriers are inevitable, so planning ahead can help create alternative options for any expected and unexpected situations that arise. Common barriers experienced by individuals experiencing chronic pain are the pain itself, poor sleep, depression, anxiety, fearavoidance beliefs, and feeling unsure about how to start and whether success is possible (Ambrose & Golightly, 2015). Additionally, fear for safety and worry about additional injury can add to the fear-avoidance cycle. Talking to a healthcare professional can help alleviate these concerns. In addition, Table 1 below lists common worries and barriers along with suggestions for overcoming them.
Summary
To review, chronic pain takes a major toll on health in the U.S. For example, fear of pain and injury prevents individuals with chronic pain from engaging in activity. Studies suggest that physical activity can be safe for people who suffer from chronic pain and can actually reduce the pain that is experienced long-term. It is important to be careful, consult experts on safety, and pace the activity in a way that avoids overdoing. Following the simple guidelines and suggestions in this fact sheet can lead to greater confidence in movement and reduced discomfort for chronic pain sufferers.
Table 1. Common Barriers to Physical Activity and Suggested Responses
| Obstacle | Try This |
|---|---|
| I don’t have time to be physically active. | Monitor your daily activities for one week. Identify at least three 30-minute time slots you could use for physical activity. Select activities that you can fit into your home or work routine. |
| I don’t have anyone to go with me. | Develop new friendships with physically active people. Join a group, such as the YMCA or a hiking club. |
| Friends or family don’t share my interest in physical activity. | Explain your fitness goals to them and ask for their support. Invite them to participate in an activity with you. |
| I’m so tired when I get home from work. |
Schedule physical activity for times in the day or week when you feel energetic. |
| Sometimes I don’t feel motivated. |
Write activities down in a calendar and check them off as you do them. If your friends and family are involved, motivate one another and hold each other accountable |
| I have so much on my “to do” list already; how can I do physical activity too? |
Plan ahead. Make physical activity a regular part of your daily or weekly schedule by writing it on your calendar. Keep the appointment with yourself. |
| I’ll probably hurt myself if I try to be more physically active. |
Consult educational material or visit with a health professional to learn how to exercise appropriately for your age, fitness level, skill level, and health status. |
| I’m not coordinated. I can’t learn something new at my age! |
Skip the dance classes if they require coordination; choose activities such as walking or biking instead. |
| My job requires me to be on the road; it’s impossible for me to exercise. |
Stay in places with swimming pools or exercise facilities. Find an exercise you enjoy and be sure you can access it on a mobile device wherever you are, or take small equipment with you, such as a jump rope and resistance bands. |
| I have small children, and it’s impossible to have time to myself for exercise. |
Trade babysitting with a friend, neighbor, or family member who also has small children. As children get older, family bike rides or walks might be another option. |
| There is a lack of resources or equipment. |
Choose activities that are low or no-cost and ones that don’t need special equipment. Identify inexpensive and convenient resources in your community, such as parks and wellness programs. Many activities require no equipment or cost very little; shop around for the best price and lower-cost alternatives. |
Note. These ideas are adapted from the CDC (2021) and the American Heart Association (2019).
References
- Ambrose, K. R., & Golightly, Y. M. (2015). Physical exercise as non-pharmacological treatment of chronic pain: Why and when. Best Practice & Research Clinical Rheumatology, 29(1), 120–130. https://doi.org/10.1016/j.berh.2015.04.022
- American College of Sports Medicine (2019). Selecting the right fitness facility for you. Retrieved April 22, 2021, from https://www.acsm.org/docs/default-source/files-for-resource-library/selecting-the-right-fitnessfacility.pdf?sfvrsn=234d6f96_4
- American Council on Exercise (2009a). How to choose a health club. Retrieved April 22, 2021, from https://www.acefitness.org/education-and-resources/lifestyle/blog/6620/how-to-choose-a-health-club/
- American Council on Exercise (2009b). How to choose the right personal trainer. Retrieved April 22, 2021, from https://www.acefitness.org/education-and-resources/lifestyle/blog/6624/how-to-choose-the-rightpersonal-trainer/
- American Heart Association (2018). Breaking down barriers to fitness. Retrieved April 22, 2021, from https://www.heart.org/en/healthy-living/fitness/getting-active/breaking-down-barriers-to-fitness
- Amtmann, D., Cook, K., Jensen, M., Chen, W., Choi, S., Revicki, D., Cella, D., Rothrock, N., Keefe, F., Callahan, L., & Lai, J. (2010, Jul). Development of a PROMIS item bank to measure pain interference. Pain, 150(1), 173-182. https://doi.org/10.1016/j.pain.2010.04.025
- Belavy, D. L., Van Oosterwijck, J., Clarkson, M., Dhondt, E., Mundell, N. L., Miller, C. T., & Owen, P. J. (2021).
Pain sensitivity is reduced by exercise training: Evidence from a systematic review and meta-analysis. Neuroscience and Biobehavioral Reviews, 120, 100–108. https://doi.org/10.1016/j.neubiorev.2020.11.012 - Björnsdóttir, S. V., Jónsson, S. H., & Valdimarsdóttir, U. A. (2013). Functional limitations and physical symptoms of individuals with chronic pain. Scandinavian Journal of Rheumatology, 42(1), 59–70. https://doi.org/10.3109/03009742.2012.697916
- Bredin, S. S., Gledhill, N., Jamnik, V. K., & Warburton, D. E. (2013). PAR-Q+ and ePARmed-X+: new risk stratification and physical activity clearance strategy for physicians and patients alike. Canadian Family Physician Medecin de Famille Canadien, 59(3), 273–277.
- Breivik, H., Borchgrevink, P. C., Allen, S. M., Rosseland, L. A., Romundstad, L., Hals, E. K., Kvarstein, G., & Stubhaug, A. (2008). Assessment of pain. British Journal of Anaesthesia, 101(1), 17–24. https://doi.org/10.1093/bja/aen103
- Canadian Society for Exercise Physiology (2021). Pre-Screening for physical activity: Get active questionnaire. https://store.csep.ca/pages/getactivequestionnaire
- Centers for Disease Control and Prevention (2021). Should I take precautions before becoming more active? Retrieved April 22, 2021, from https://www.cdc.gov/healthyweight/physical_activity/getting_started.html
- Center for Disease Control and Prevention. (n.d.). Benefits of physical activity. Retrieved April 22, 2021, from https://www.cdc.gov/physicalactivity/basics/pa-health/index.htm
- Dueñas, M., Ojeda, B., Salazar, A., Mico, J. A., & Failde, I. (2016). A review of chronic pain impact on patients, their social environment and the health care system. Journal of Pain Research, 9, 457–467. https://doi.org/10.2147/JPR.S105892
- Dunstan, D. W., Kingwell, B. A., Larsen, R., Healy, G. N., Cerin, E., Hamilton, M. T., Shaw, J. E., Bertovic, D. A., Zimmet, P. Z., Salmon, J. & Owen, N. (2012). Breaking Up Prolonged Sitting Reduces Postprandial Glucose and Insulin Responses. Diabetes Care, 35(5), 976–983; DOI: 10.2337/dc11-1931
- Dunstan, D. W., Kingwell, B. A., Larsen, R., Healy, G. N., Cerin, E., Hamilton, M. T., Shaw, J. E., Bertovic, D. A., & Gilmour H. (2015). Chronic pain, activity restriction and flourishing mental health. Health Reports, 26(1), 15–22.
- Geneen, L., Moore, R., Clark, C., Martin D., Colvin, L., & Smith, B. (2017). Physical activity and exercise for chronic pain in adults: An overview of Cochrane Reviews. Cochrane Database of Systematic Reviews, 2. doi:10.1002/14651858.CD011279.pub3
- Grady, P. A., & Gough, L. L. (2014). Self-management: a comprehensive approach to management of chronic conditions. American Journal of Public Health, 104(8), e25–e31. https://doi.org/10.2105/AJPH.2014.302041
- Harvard Health Publishing (2014). Get on your feet: 8 creative ways to avoid too much sitting. Harvard Women’s Health Watch. https://www.health.harvard.edu/staying-healthy/get-on-your-feet-8-creative-waysto-avoid-too-much-sitting
- Harvard Medical School (2012). Do you need to see a doctor before starting your exercise program? Harvard Health Publishing Healthbeat. https://www.health.harvard.edu/healthbeat/do you-need-to-see-a-doctorbefore-starting-your-exercise-program
- Harvard Medical School (2018). Rethinking the 30-minute workout. Harvard Health Publishing Harvard Men’s Health Watch. Retrieved April 22, 2021, from: https://www.health.harvard.edu/staying-healthy/rethinkingthe-30-minute-workout
- Henschke, N., Kamper, S. J., & Maher, C. G. (2015, January). The epidemiology and economic consequences of pain. In Mayo Clinic Proceedings 90(1), 139–147. Elsevier.
- Larsen, R., Kingwell, B., Sethi, P., Cerin, E., Owen, N., & Dunstan, D. (2014). Breaking up prolonged sitting reduces resting blood pressure in overweight/obese adults. Nutrition, Metabolism, and Cardiovascular Diseases, 24(9), 976–982. DOI: https://doi.org/10.1016/j.numecd.2014.04.011
- Law, L. F., & Sluka, K. A. (2017). How does physical activity modulate pain? Pain, 158(3), 369–370. https://doi.org/10.1097/j.pain.0000000000000792
- Loos, H., Sulzer, S. H., & Atismé, K. (n.d.). Exercise tips for chronic pain management. Utah State University Extension. Retrieved March 13, 2021, from https://extension.usu.edu/heart/files/exercisetipsforchronicpainmanagement.pdf
- Mackichan, F., Adamson, J., & Gooberman-Hill, R. (2013). 'Living within your limits': Activity restriction in older people experiencing chronic pain. Age and Ageing, 42(6), 702–708. https://doi.org/10.1093/ageing/aft119
- National Institute on Aging. (n.d.) Exercising with chronic conditions. National Institute of Health. U.S. Department of Health and Human Services. https://www.nia.nih.gov/health/exercising-chronic conditions
- Rainville, J., Hartigan, C., Martinez, E., Limke, J., Jouve, C., Finno, M. (2004). Exercise as a treatment for chronic low back pain. The Spine Journal, 4(1), 106–115.
- Rall, L. C., & Roubenoff, R. (2011). Benefits of exercise for patients with rheumatoid arthritis. Nutrition in Clinical Care, 3(4), 209–215.
- Thomas, E., Peat, G., Harris, L., Wilkie, R., & Croft, P. R. (2004). The prevalence of pain and pain interference in a general population of older adults: Cross-sectional findings from the North Staffordshire Osteoarthritis Project (NorStOP). Pain, 110(1-2), 361–368. https://doi.org/10.1016/j.pain.2004.04.017
- Thorp, A., Kingwell, B., Owen, N., & Dunstan, D. (2014). Breaking up workplace sitting time with intermittent standing bouts improves fatigue and musculoskeletal discomfort in overweight/obese office workers. Occupational and Environmental Medicine, 71(11), 765–771. DOI: 10.1136/oemed-2014-102348
- Treede, R., D., Rief, W., Barke, A., Aziz, Q., Bennett, M. I., Benoliel, R., Cohen, M., Evers, S., Finnerup, N. B., First, M. B., Giamberardino, M. A., Kaasa, S., Kosek, E., Lavand'homme, P., Nicholas, M., Perrot, S., Scholz, J., Schug, S., Smith, B.… Wang, S. (2015). A classification of chronic pain for ICD-11. Pain, 156(6), 1003–1007. https://doi.org/10.1097/j.pain.0000000000000160
- University of Iowa Hospitals and Clinics. (2018, March). Exercise to treat chronic pain [Video]. YouTube. https://uihc.org/health-topics/exercise-treat-chronic-pain
- U.S. Department of Health and Human Services. (2018). Physical activity guidelines for Americans, (2nd ed.) U.S. Department of Health and Human Services. https://health.gov/sites/default/files/2019- 09/Physical_Activity_Guidelines_2nd_edition.pdf
- Vina, J., Sanchis‐Gomar, F., Martinez‐Bello, V., & Gomez‐Cabrera, M. C. (2021, September 1). Exercise acts as a drug; the pharmacological benefits of exercise. British Journal of Pharmacology, 167(1), 1–2.
- Warburton, D., Jamnik, V. K., Bredin, S. D., McKenzie, D. C., Stone, J., Shephard, R. J., & Gledhill, N. (2011). Evidence-based risk assessment and recommendations for physical activity clearance: An introduction. Applied Physiology, Nutrition, and Metabolism, 36(S1), S1–S2. https://doi.org/10.1139/h11-060
- Zimmet, P. Z., Salmon, J., & Owen, N. (2012). Breaking up prolonged sitting reduces postprandial glucose and insulin responses. Diabetes Care, 35(5), 976–983. DOI: 10.2337/dc11-1931
Authors
Maren Wright Voss, Sc.D.; Mateja Savoie-Roskos, Ph.D.; Casey Coombs, M.S.; Gabriela Murza, M.S.; Cindy Nelson, M.S.; Elise Withers, B.S.
Related Research